Shin Splints
Shin Splints (Medial Tibial Stress Syndrome) & Compartment Syndrome
Shin splints is the catch-all term for lower leg pain. Typically the pain occurs below the knee either on the front outside part of the leg (anterior shin splints), or the inside of the leg (medial shin splints). Shin splints are the bane of many athletes, runners, tennis players, and even dancers. They often plague beginning runners who do not build their mileage gradually enough, or seasoned runners who abruptly change their workout regimen, suddenly adding too much mileage or switching from running on flat surfaces to hills.
The nature of shin splints, also known as medial tibial stress syndrome (MTSS), most often can be captured in four words: too much, too soon.
Shin pain doesn’t always mean you have shin splints. It might be a sign of some other problem. The following are two conditions that are sometimes mistakenly diagnosed as shin splints.
Pain on the anterior (outside) part of the lower leg may be compartment syndrome—a swelling of muscles within a closed compartment—which creates pressure. To diagnose this condition, special techniques are used to measure the amount of pressure. Surgical “decompression” can be required. The symptoms of compartment syndrome include leg pain, unusual nerve sensations, and eventually muscle weakness.
Pain in the lower leg could also be a stress fracture (an incomplete crack in the bone), which is a far more serious injury than shin splints. A bone scan is the definitive tool for diagnosing a stress fracture. However, there are clues you can look for that will signal whether or not you should get a bone scan.
The pain of shin splints is also more generalized than that of a stress fracture. Press your fingertips along your shin, and if you can find a definite spot of sharp pain, it’s a sign of a stress fracture. Additionally, stress fractures often feel better in the morning because the bone has rested all night; they often feel worse in the morning because the soft tissue tightens overnight. Shin splints are also at their most painful when you forcibly try to lift your foot up at the ankle and flex your foot.
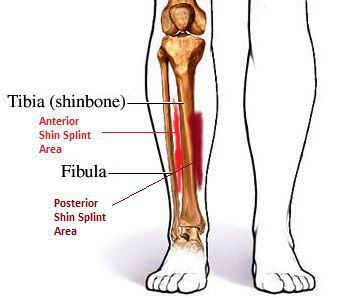
Common causes of shin splints
There can be a number of factors at work, such as over pronation (a frequent cause of medial shin splints), inadequate stretching, worn shoes, or excessive stress placed on one leg or one hip from running on cambered roads or always running in the same direction on a track. Typically, one leg is involved and it is almost always the runner’s dominant one. If you’re right-handed, you’re usually right-footed as well, and that’s the leg that’s going to hurt.
The most common site for shin splints is the medial area (the inside of the shin). Anterior shin splints (toward the outside of the leg) usually result from an imbalance between the calf muscles and the muscles in the front of your leg, and often afflict beginners who either have not yet adjusted to the stresses of running or are not stretching enough.
But what exactly is a shin splint? There’s no end-all consensus among sports scientists, and theories have included small tears in the muscle that’s pulled off the bone, an inflammation of the periosteum [a thin sheath of tissue that wraps around the tibia, or shin bone], an inflammation of the muscle, or some combination of these. Fortunately, medical experts agree on how to treat them.
Treatment of shin splints

Experts agree that when shin splints strike you should stop running completely or decrease your training depending on the extent and duration of pain. Then, as a first step, ice your shin to reduce inflammation. Here are some other treatments you can try:
Gently stretch your Achilles if you have medial shin splints, and your calves if you have anterior shin splints. Also, try this stretch for your shins: Kneel on a carpeted floor, legs and feet together and toes pointed directly back. Then slowly sit back onto your calves and heels, pushing your ankles into the floor until you feel tension in the muscles of your shin. Hold for 10 to 12 seconds, relax and repeat.
In a sitting position, trace the alphabet on the floor with your toes. Do this with each leg. Or alternate walking on your heels for 30 seconds with 30 seconds of regular walking. Repeat four times. These exercises are good for both recovery and prevention. Try to do them three times a day.
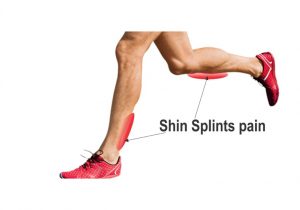
If you continue running, wrap your leg before you go out. Use either tape or an Ace bandage, starting just above the ankle and continuing to just below the knee. Keep wrapping your leg until the pain goes away, which usually takes three to six weeks.
Consider cross-training for a while to let your shin heal. Swim, run in the pool or ride a bike.
When you return to running, increase your mileage slowly, no more than 10 percent weekly.
Make sure you wear the correct running shoes for your foot type specifically, overpronators should wear motion-control shoes. Severe overpronators may need orthotics to correct poor biomechanics and prevent muscle overuse.
Have two pairs of shoes and alternate wearing them to vary the stresses on your legs.
Avoid hills and excessively hard surfaces until shin pain goes away completely, then re-introduce them gradually to prevent a recurrence.
If you frequently run on roads with an obvious camber, run out and back on the same side of the road. Likewise, when running on a track, switch directions.
If you are prone to developing shin splints, stretch your calves and Achilles regularly as a preventive measure.
Swiss DolorClast® : Medial Tibial Stress Syndrome – (RSWT®) Radial Shock Wave Therapy
Podiatrists at The Foot and Ankle Clinic have vast experience in diagnosing and treating Shin Splints. Typically this treatment is very successful but involves a multifactorial approach.
At the Foot and Ankle Clinic our highly qualified team of Podiatrists are all members of the Australian Podiatry Association and offer a combined 50 years’ experience. They are trained to diagnose and effectively treat shin splints via a range of treatments.
Put your feet in our hands! See us today in Chadstone, East Bentleigh, Moe, Sale, Traralgon, Warragul & Online Store and Retail Enquiries. NO REFERRAL NEEDED!.


